I know, I know. When you see that question on an application, you want to answer ‘yes,’ but you’re only given the choice of male or female. Well, at least that’s my experience. Okay, got that out of the way.
 Way back in 2011, the following was included in my first Chronic Kidney Disease book, What Is It and How Did I Get It? Early Stage Chronic Kidney Disease. This was way before the website, Facebook page, the blog, the Instagram, Pinterest, Twitter, and LinkedIn accounts. Way before the articles, radio shows, and interviews, book signings, and talks about CKD. Come to think of it, this was way before SlowItDownCKD was born.
Way back in 2011, the following was included in my first Chronic Kidney Disease book, What Is It and How Did I Get It? Early Stage Chronic Kidney Disease. This was way before the website, Facebook page, the blog, the Instagram, Pinterest, Twitter, and LinkedIn accounts. Way before the articles, radio shows, and interviews, book signings, and talks about CKD. Come to think of it, this was way before SlowItDownCKD was born.
I haven’t found too much about sex that’s different from the problems of non-CKD patients although with this disease there may be a lower sex drive accompanied by a loss of libido and an inability to ejaculate. Usually, these problems start with an inability to keep an erection as long as usual. The resulting impotency has a valid physical, psychological or psycho-physical cause.

Some of the physical causes of impotence, more recently referred to as Erectile Dysfunction [E.D.] for a CKD patient could be poor blood supply since there are narrowed blood vessels all over the body. Or maybe it’s leaky blood vessels. Of course, it could be a hormonal disturbance since the testicles may be producing less testosterone and the kidneys are in charge of hormones….
While E.D. can be caused by renal disease, it can also be caused by diabetes and hypertension. All three are of importance to CKD patients. Sometimes, E.D. is caused by the medications for hypertension, depression and anxiety. But, E.D. can also be caused by other diseases, injuries, surgeries, prostate cancer or a host of other conditions and bodily malfunctions. Psychologically, the problem may be caused by stress, low self-esteem, even guilt to name just a few  of the possible causes….
of the possible causes….
Women with CKD may also suffer from sexual problems, but the causes can be complicated. As with men, renal disease, diabetes and hypertension may contribute to the problem. But so can poor body image, low self-esteem, depression, stress and sexual abuse. Any chronic disease can make a man or a woman feel less sexual….
Common sense tells us that sex or intimacy is not high on your list of priorities when you’ve just been recently diagnosed….
Sometimes people with chronic diseases can be so busy being the patient that they forget their partners have needs, too. And sometimes, remembering to stay close, really close as in hugging and snuggling, can be helpful….
Well, what’s changed since I was writing What Is It and How Did I Get It? Early Stage Chronic Kidney Disease? in 2010?
The National Kidney Foundation at https://www.kidney.org/atoz/content/sexuality now includes the following on their website:
It’s important to remember that people with kidney failure can have healthy marriages and meaningful relationships. They can fall in love, care for families, and be sexual. Staying intimate with those you love is important. It’s something everyone needs.
Many people think that sexuality refers only to sexual intercourse. But sexuality includes many things, like touching, hugging, or kissing. It includes how you feel about yourself, how well you communicate, and how willing you are to be close to someone else.
There are many things that can affect your sexuality if you have kidney disease or kidney failure — hormones, nerves, energy levels, even medicine. But there are also things you and your healthcare team can do to deal with these changes. Don’t be afraid to ask questions or get help from a healthcare professional.
DaVita at https://www.davita.com/kidney-disease/overview/living-with-ckd/sexuality-and-chronic-kidney-disease/e/4895 also offers advice:
Once again, it’s important to remember, you are not alone.
There are no limits with regard to sexual activities you may engage in as a patient with renal disease, as long as activity does not place pressure or tension on the access site, causing damage. (Me: This is for advanced CKD.)
If you are sexually active, practicing safe sex and/or using birth control are needed, even if you think you may be physically unable to have children.
Activities such as touching, hugging and kissing provide feelings of warmth and closeness even if intercourse is not involved. Professional sex therapists can recommend alternative methods as well.
Keeping an open mind and having a positive attitude about yourself and your sexuality may lower the chances of having sexual problems.
There are both medical and emotional causes for sexual dysfunction. The reason for your dysfunction can be determined through a thorough physical exam in addition to an assessment of your emotional welfare and coping skills.
Relaxation techniques, physical exercise, writing in a journal and talking to your social worker or a therapist can help you to feel better about your body image and/or sexual dysfunction.
Resuming previous activities, such as dining out or traveling, as a couple or single adult, can be helpful.
Provide tokens of affection or simple acts of kindness to show you care.
Communicate with your partner or others about how you feel.
 According to the Kidney Foundation of Canada at file:///C:/Users/Owner/AppData/Local/Packages/Microsoft.MicrosoftEdge_8wekyb3d8bbwe/TempState/Downloads/Sexuality%20and%20CKD.pdf, these may be the causes of sexual problems in CKD.
According to the Kidney Foundation of Canada at file:///C:/Users/Owner/AppData/Local/Packages/Microsoft.MicrosoftEdge_8wekyb3d8bbwe/TempState/Downloads/Sexuality%20and%20CKD.pdf, these may be the causes of sexual problems in CKD.
Fatigue is a major factor. Any chronic illness is tiring, and chronic kidney disease, which is often accompanied by anemia and a demanding treatment, practically guarantees fatigue.
Depression is another common issue. Almost everyone experiences periods of depression, and one of the symptoms of depression is loss of interest in sexual intimacy.
Medications can also affect one’s ability or desire to have intercourse. Since there may be other medications which are just as effective without the side effect of loss of sexual function or desire, talk to your doctor about your pills.
Feelings about body image Having a peritoneal catheter, or a fistula or graft, may cause some people to avoid physical contact for fear of feeling less attractive or worrying about what people think when they look at them. (Me: Again, this is for late stage CKD.)
Some diseases, such as vascular disease and diabetes, can lead to decreased blood flow in the genital area, decreased sexual desire, vaginal dryness and impotence.
It looks like the information about CKD and sexuality hasn’t changed that much, but it does seem to be more available these days.
Until next week,
Keep living your life!



 No, that’s not the result of misplacing my fingers on the keyboard. According to
No, that’s not the result of misplacing my fingers on the keyboard. According to 


 “Your immune system is a complex network of cells, tissues, and organs that work together to defend against germs. It helps your body to recognize these ‘foreign’ invaders. Then its job is to keep them out, or if it can’t, to find and destroy them.”
“Your immune system is a complex network of cells, tissues, and organs that work together to defend against germs. It helps your body to recognize these ‘foreign’ invaders. Then its job is to keep them out, or if it can’t, to find and destroy them.”

 “Constipation can be caused by a variety of medications. These medications affect the nerve and muscle activity in the large intestine (colon) and may also bind intestinal liquid. This may result in slowed colonic action (slow and/or difficult passing of stool).”
“Constipation can be caused by a variety of medications. These medications affect the nerve and muscle activity in the large intestine (colon) and may also bind intestinal liquid. This may result in slowed colonic action (slow and/or difficult passing of stool).”

 “adjective
“adjective

 Do Not Smoke
Do Not Smoke

 given my work and experience on this topic.
given my work and experience on this topic.
 “I’d always thought that AKI and CKD were separate issues and I’ll bet you did, too. But Dr. L.S. Chawla and his co-writers based the following conclusion on the labor of epidemiologists and others. (Note: Dr. Chawla et al wrote a review article in the New England Journal of Medicine in 2014.)
“I’d always thought that AKI and CKD were separate issues and I’ll bet you did, too. But Dr. L.S. Chawla and his co-writers based the following conclusion on the labor of epidemiologists and others. (Note: Dr. Chawla et al wrote a review article in the New England Journal of Medicine in 2014.)
 One thing Dana asked that made me stop cold is “How do you cope with the inevitable aspects?” They are not inevitable, Dana. I am a lay person who has managed to keep my CKD at stage 3 for 11 years. I am also not a magician. What I am is someone who follows the guidelines for keeping my kidneys as healthy as possible.
One thing Dana asked that made me stop cold is “How do you cope with the inevitable aspects?” They are not inevitable, Dana. I am a lay person who has managed to keep my CKD at stage 3 for 11 years. I am also not a magician. What I am is someone who follows the guidelines for keeping my kidneys as healthy as possible.
 We all know diabetes raises your risk of developing Chronic Kidney Disease. But why? What’s the mechanism behind the fact? As far as I’m concerned, it’s time to find out.
We all know diabetes raises your risk of developing Chronic Kidney Disease. But why? What’s the mechanism behind the fact? As far as I’m concerned, it’s time to find out.

 “Dapagliflozin is used along with diet and exercise, and sometimes with other medications, to lower blood sugar levels in patients with type 2 diabetes (condition in which blood sugar is too high because the body does not produce or use insulin normally). Dapagliflozin is in a class of medications called sodium-glucose co-transporter 2 (SGLT2) inhibitors. It lowers blood sugar by causing the kidneys to get rid of more glucose in the urine. Dapagliflozin is not used to treat type 1 diabetes (condition in which the body does not produce insulin and, therefore, cannot control the amount of sugar in the blood) or diabetic ketoacidosis (a serious condition that may develop if high blood sugar is not treated).
“Dapagliflozin is used along with diet and exercise, and sometimes with other medications, to lower blood sugar levels in patients with type 2 diabetes (condition in which blood sugar is too high because the body does not produce or use insulin normally). Dapagliflozin is in a class of medications called sodium-glucose co-transporter 2 (SGLT2) inhibitors. It lowers blood sugar by causing the kidneys to get rid of more glucose in the urine. Dapagliflozin is not used to treat type 1 diabetes (condition in which the body does not produce insulin and, therefore, cannot control the amount of sugar in the blood) or diabetic ketoacidosis (a serious condition that may develop if high blood sugar is not treated).


 Let’s go to my favorite dictionary, the Merriam-Webster Dictionary at
Let’s go to my favorite dictionary, the Merriam-Webster Dictionary at 


 HERE’S THE STORY
HERE’S THE STORY
 What does CKD research typically focus on?
What does CKD research typically focus on? 
 As most of you know, I am extremely protective of my kidneys. When I was first diagnosed with Chronic Kidney Disease 11 years ago, my eGFR was only 39. Here’s a quick reminder of what the eGFR is from my first CKD book,
As most of you know, I am extremely protective of my kidneys. When I was first diagnosed with Chronic Kidney Disease 11 years ago, my eGFR was only 39. Here’s a quick reminder of what the eGFR is from my first CKD book, 
 National Kidney Month is just flying by. This is actually the last week and I doubt I’ll be able to post the rest of the 1in9 chapter before next month. But then again, it’s always Kidney Month for those of us with Chronic Kidney Disease. By the way, thank you to the reader who made it a point of telling me she can’t wait to read the rest of the chapter. Sooooo, let’s get started!
National Kidney Month is just flying by. This is actually the last week and I doubt I’ll be able to post the rest of the 1in9 chapter before next month. But then again, it’s always Kidney Month for those of us with Chronic Kidney Disease. By the way, thank you to the reader who made it a point of telling me she can’t wait to read the rest of the chapter. Sooooo, let’s get started!

 Exercise, something I loved until my arthritis got in the way, was also important. I was a dancer. Wasn’t that enough? Uh-uh, I had to learn about cardio and strength training exercise, too. It was no longer acceptable to be pleasantly plumb. My kidneys didn’t need the extra work. Hello to weights, walking, and a stationary bike. I think I took sleep for granted before CKD, too, and I now make it a point to get a good night’s sleep. A sleep apnea device improved my sleep—and my kidney function rose.
Exercise, something I loved until my arthritis got in the way, was also important. I was a dancer. Wasn’t that enough? Uh-uh, I had to learn about cardio and strength training exercise, too. It was no longer acceptable to be pleasantly plumb. My kidneys didn’t need the extra work. Hello to weights, walking, and a stationary bike. I think I took sleep for granted before CKD, too, and I now make it a point to get a good night’s sleep. A sleep apnea device improved my sleep—and my kidney function rose. Tomorrow is Christmas and a Merry Christmas to those of you who celebrate. The day after Christmas Kwanzaa begins, so a Happy Kwanzaa to those of you who celebrate. But back to Christmas right now: today’s blog is a present to a reader who joined me way back when I first started blogging and has since become a close online friend.
Tomorrow is Christmas and a Merry Christmas to those of you who celebrate. The day after Christmas Kwanzaa begins, so a Happy Kwanzaa to those of you who celebrate. But back to Christmas right now: today’s blog is a present to a reader who joined me way back when I first started blogging and has since become a close online friend.
 “Kidney diseases or disorders can lead to high creatinine levels. Since the kidneys are the filters of wastes from the bloodstream, kidney damage means that there will be a buildup of creatinine beside other waste products in the body. Kidney conditions such as glomerulonephritis, acute tubular necrosis, kidney infection (pyelonephritis) and kidney failure can cause high creatinine levels. Reduced blood flow to the kidneys can also have a similar effect.
“Kidney diseases or disorders can lead to high creatinine levels. Since the kidneys are the filters of wastes from the bloodstream, kidney damage means that there will be a buildup of creatinine beside other waste products in the body. Kidney conditions such as glomerulonephritis, acute tubular necrosis, kidney infection (pyelonephritis) and kidney failure can cause high creatinine levels. Reduced blood flow to the kidneys can also have a similar effect. “As the blood filtering units of your body, your kidneys are prone to problems with blood circulation and blood vessels. High blood pressure and high blood sugar can place an additional strain or burden on your kidneys. People with high blood pressure and diabetes are at a higher risk for kidney disease. People with kidney disease are at higher risk for heart and blood vessel disease. If you already have heart and blood vessel disease and kidney disease, then the body’s reactions to stress can become more and more dangerous. Therefore, whether your goal is to prevent heart and/or kidney disease, or improve your health while living with heart and/or kidney disease, managing stress is an important part of maintaining your overall health.”
“As the blood filtering units of your body, your kidneys are prone to problems with blood circulation and blood vessels. High blood pressure and high blood sugar can place an additional strain or burden on your kidneys. People with high blood pressure and diabetes are at a higher risk for kidney disease. People with kidney disease are at higher risk for heart and blood vessel disease. If you already have heart and blood vessel disease and kidney disease, then the body’s reactions to stress can become more and more dangerous. Therefore, whether your goal is to prevent heart and/or kidney disease, or improve your health while living with heart and/or kidney disease, managing stress is an important part of maintaining your overall health.” the symptoms. These are the same whether you’re the patient or the caretaker. I happen to be both a CKD patient and my Alzheimer’s husband’s caretaker, although we call me his care partner as suggested by the Alzheimer’s Association.
the symptoms. These are the same whether you’re the patient or the caretaker. I happen to be both a CKD patient and my Alzheimer’s husband’s caretaker, although we call me his care partner as suggested by the Alzheimer’s Association. Today is the last day of the eight day Chanukah celebration for us and all of you who celebrate this holiday. We usually throw a blowout party for anywhere from 30 to 50 people. But just a couple of months ago, we hosted a blowout pre-wedding potluck party for my daughter and her fiancé … and it was wonderful. Yet, it was clear that we can no longer handle undertaking such large parties. I had expressed my doubts last year about how long we’d be able to keep up the Chanukah party.
Today is the last day of the eight day Chanukah celebration for us and all of you who celebrate this holiday. We usually throw a blowout party for anywhere from 30 to 50 people. But just a couple of months ago, we hosted a blowout pre-wedding potluck party for my daughter and her fiancé … and it was wonderful. Yet, it was clear that we can no longer handle undertaking such large parties. I had expressed my doubts last year about how long we’d be able to keep up the Chanukah party.

 Food and Drug Administration
Food and Drug Administration

 okay, I guess that sort of makes sense. And then, oh my, I developed diabetes. But how? I’d never questioned how that worked before, but I certainly did now.
okay, I guess that sort of makes sense. And then, oh my, I developed diabetes. But how? I’d never questioned how that worked before, but I certainly did now. Guilty on all three counts as far as symptoms. It gets worse. I uncovered this fact in
Guilty on all three counts as far as symptoms. It gets worse. I uncovered this fact in 
 I would say I’m heart… uh, kidney…broken about this development, but the truth is I’m not. I don’t like it; I don’t want it, but I can do something about it. I’d already cut out complex carbs and sugar laden foods in an abortive attempt to lose weight for my health. Well, maybe my daughter’s wedding on October 6th had something to do with that decision, too.
I would say I’m heart… uh, kidney…broken about this development, but the truth is I’m not. I don’t like it; I don’t want it, but I can do something about it. I’d already cut out complex carbs and sugar laden foods in an abortive attempt to lose weight for my health. Well, maybe my daughter’s wedding on October 6th had something to do with that decision, too.

 suggesting I do so for years, but I’m not a joiner. Let’s change that; I wasn’t a joiner. The AAKP conference made the difference.
suggesting I do so for years, but I’m not a joiner. Let’s change that; I wasn’t a joiner. The AAKP conference made the difference.
 AAKP has grown into a nationally recognized patient organization that reaches over 1 million people yearly. It remains dedicated to providing patients with the education and knowledge necessary to ensure quality of life and quality of health.”
AAKP has grown into a nationally recognized patient organization that reaches over 1 million people yearly. It remains dedicated to providing patients with the education and knowledge necessary to ensure quality of life and quality of health.”

 When I was a little girl, I liked to listen to my father whistle ‘All of Me,’ written by Marks and Simon in 1931 when Charlie, my father, was just 16. Only a few years later, it became a sort of love language for my mother and him. Enter a former husband of my own and my children. When my folks visited from Florida and my then husband’s side of the family journeyed over to Staten Island from Brooklyn to visit them, they all sang the song with great emotion. (By then, Bell’s palsy had robbed my father of the ability to whistle.)
When I was a little girl, I liked to listen to my father whistle ‘All of Me,’ written by Marks and Simon in 1931 when Charlie, my father, was just 16. Only a few years later, it became a sort of love language for my mother and him. Enter a former husband of my own and my children. When my folks visited from Florida and my then husband’s side of the family journeyed over to Staten Island from Brooklyn to visit them, they all sang the song with great emotion. (By then, Bell’s palsy had robbed my father of the ability to whistle.)
 Better Information
Better Information
 decline in our kidney function. I maintain that if only my primary care physician had told me when he first noticed that 39% GFR, maybe I wouldn’t be in stage 3 of 5. Maybe those now on dialysis or searching for a transplant wouldn’t be in the position they are, either.
decline in our kidney function. I maintain that if only my primary care physician had told me when he first noticed that 39% GFR, maybe I wouldn’t be in stage 3 of 5. Maybe those now on dialysis or searching for a transplant wouldn’t be in the position they are, either.
 The literature suggests early nephrologist involvement improves long-term outcomes. Proactive primary care offers longitudinal guidance for making the enormous lifestyle changes in diet, exercise, stress management, hydration, sleep and toxic exposures, while offering psychological counseling that is required to achieve such changes. The cross-over benefits for patients’ other diagnoses is well known.
The literature suggests early nephrologist involvement improves long-term outcomes. Proactive primary care offers longitudinal guidance for making the enormous lifestyle changes in diet, exercise, stress management, hydration, sleep and toxic exposures, while offering psychological counseling that is required to achieve such changes. The cross-over benefits for patients’ other diagnoses is well known. surgeries, travel and stress — need to grasp a breadth of nephrology basics. Our patients with CKD are at increased risk of acute kidney injury. Astute protection means we save nephrons. This author would welcome renal rotations at all levels of medical training, with a facet of focus on longitudinal outpatient, early and moderate CKD care. This vision of collaboration, with a commitment to early diagnosis and intervention, offers the opportunity to learn how to guide patients to a less inflammatory lifestyle.
surgeries, travel and stress — need to grasp a breadth of nephrology basics. Our patients with CKD are at increased risk of acute kidney injury. Astute protection means we save nephrons. This author would welcome renal rotations at all levels of medical training, with a facet of focus on longitudinal outpatient, early and moderate CKD care. This vision of collaboration, with a commitment to early diagnosis and intervention, offers the opportunity to learn how to guide patients to a less inflammatory lifestyle.


 I was going to give you my take on researching when I stumbled across Dr. Alicia White’s piece on the United Kingdom’s National Health Services site at
I was going to give you my take on researching when I stumbled across Dr. Alicia White’s piece on the United Kingdom’s National Health Services site at 
 Also, it’s important that the control group is as similar to the treated/exposed group as possible. The best way to achieve this is to randomly assign some people to be in the treated/exposed group and some people to be in the control group. This is what happens in a randomised controlled trial (RCT) and is why RCTs are considered the “gold standard” for testing the effects of treatments and exposures. … Without either, retain some healthy scepticism.
Also, it’s important that the control group is as similar to the treated/exposed group as possible. The best way to achieve this is to randomly assign some people to be in the treated/exposed group and some people to be in the control group. This is what happens in a randomised controlled trial (RCT) and is why RCTs are considered the “gold standard” for testing the effects of treatments and exposures. … Without either, retain some healthy scepticism.
 What is an endoscopy, you ask. According to the Mayo Clinic at
What is an endoscopy, you ask. According to the Mayo Clinic at 




 According to the Kidney Foundation of Canada at
According to the Kidney Foundation of Canada at 

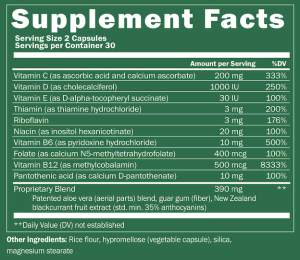
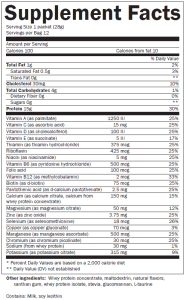
 Learning to read a Nutrition Facts label is a must if the doctor wants to do all he or she can to help the patient slow down – and sometimes halt – the progression of kidney disease. It is important to remember that in the earlier stages of kidney disease, the diet may not be as strict – but if progression of the disease is noted, then dietary modifications are more stringent and frequent laboratory tests may need to be performed to assess progress.
Learning to read a Nutrition Facts label is a must if the doctor wants to do all he or she can to help the patient slow down – and sometimes halt – the progression of kidney disease. It is important to remember that in the earlier stages of kidney disease, the diet may not be as strict – but if progression of the disease is noted, then dietary modifications are more stringent and frequent laboratory tests may need to be performed to assess progress. over the counter medications that may harm your kidneys such as Advil, Motrin, Aleve, Ibuprofen, Celebrex, Prilosec, herbal remedies, etc. I encourage all patients to memorize their medications and keep a list with them at all times. Remember that all medications are prescribed because the benefit to the patient outweighs the risk and no medication is entirely safe; therefore, it should be taken as prescribed and any side effects reported to your doctor. You should not take any new medicine unless it has been cleared by your kidney specialist.
over the counter medications that may harm your kidneys such as Advil, Motrin, Aleve, Ibuprofen, Celebrex, Prilosec, herbal remedies, etc. I encourage all patients to memorize their medications and keep a list with them at all times. Remember that all medications are prescribed because the benefit to the patient outweighs the risk and no medication is entirely safe; therefore, it should be taken as prescribed and any side effects reported to your doctor. You should not take any new medicine unless it has been cleared by your kidney specialist.